An in-depth look at the pathophysiology and treatment of Osgood-Schlatter Disease - Part C
Part C: Exercise Program Prescription
Client Screening
HistoryThe first step and perhaps the most revealing component of the primary assessment is history of the client. The primary goal of the history assessment, is to determine the mechanism and site of injury. (Perrin, D.H., 1999) This may be helpful in establishing the diagnosis, the severity of the injury, and may potentially reveal some predisposing factors (John F. DiFiori, 1999). Questions during the screening should be focused around establishing the time frame between the first onset of symptoms and present, the level of activity several weeks prior to first onset symptom, with focus on, type of activity (sport), training frequency, duration, intensity, and mode of exercise (John F. DiFiori, 1999). Another very important area of focus is age, and changes in height, and weight, in the recent months or weeks, as a means of establishing possible recent growth spurts. Injuries that occur without obvious training changes may be related to the musculoskeletal changes associated with accelerated growth (John F. DiFiori, 1999). A previous history of injuries should be gathered in order to establish possible reasons for potential weakness and prior deficiencies. Along with past history injuries, the patient should be asked to describe the location and quality of pain with specific actions, motions, and skills that bring on pain, and when does the pain most often occur with activity (John F. DiFiori, 1999). Pain that occurs at end of activity and resolves before the next training session is usually a sign of relatively mild injury; pain that occurs during activity and impairs performance is more sever (John F. DiFiori, 1999). The possibility of occult tumours or rheumatologic conditions in young athletes with chronic pain symptoms should always be considered. (John F. DiFiori, 1999)The next step is to visually inspect the injury (Perrin, D.H., 1999). Of special interest during the this stage is to observe abnormalities in gait, bilateral comparison such patellar position, obvious skeletal and joint deformities such as enlargement or prominence of tibial tubercle, muscle atrophy, signs of inflammation, swelling, skin appearance, discoloration, signs of trauma, and limitations in motion and weight bearing,(Perrin, D.H., 1999, Munisha Mehra Bhatia, 2004)
Physical Examination
The first part of the physical examination is palpation of the injury site (Perrin, D.H., 1999). The exam should proceed from the ground-up, beginning with foot and ankle alignment, and continuing proximally (John F. DiFiori, 1999). The purpose of this is to identify the exact anatomical structures involved (Perrin, D.H., 1999). Important anatomical structure that require examination are superior and inferior aspects of the patellar tendon and patellar poles (In order to eliminate potential differential diagnosis that might have been missed, such as Sindling-Larson-Johansson syndrome, patellofemoral syndrome, patellar fractures, and patellar tendonitis (Eric J. Wall, 1998, Walter L. Calmbach & Mark Hutchens, 2003), the tibial tubercle, and surrounding musculature. With palpation it should also be note if there is presence of excessive heat due to inflammation of patellar tendon, volume and consistency of swelling, which will indicate effusion or hemarthrsosis, and calcification (a sign of possible ossicle formation) (Perrin, D.H, 1999, James F. Dunn Jr., 1990). Palpation 2in below the patellar, which demonstrate tenderness and pain, is a positive diagnostic sign of OSD, along with any deformity of the tibial tuberosity (Munisha Mehra Bhatia, 2004)
The next step in the physical examination is motion assessment. The goal of this step is to determine the nature of the anatomical structures involved or associated with the extensor mechanism, and the knee mechanics (Perrin, D.H, 1999, G.S Dowd, 1996). Special attention should be paid to normal quadriceps (primarily rectus femoris), hamstring, calf and hip flexibility in active and passive range motion (McKesson Health Solutions, 2004). Because in most OSD patients the quadriceps and the hamstrings are tight, the main aim of a stretching program is to establish an H/Q ratio of 0.6, which is believed to be best, in terms of injury prevention and rehabilitation (Rosalind Coombs and Gerard Garbutt, 2002). Quadriceps flexibility is tested by a prone knee flexion test, and with the Ely test (Deborah Roche, 2005, Gregory S. Kolt & Lynn Snyder-Mackler, 2003). Hamstrings can be testes with a straight leg raise test, and a sit and reach (Deborah Roche, 2005). I believe that it would be also wise to test hip flexion also, as the rectus femoris is involved in hip flexion ,thus during hip flexion while standing, its pulls on the tibial tuberosity, and tight and weak hip flexors will mean the rectus femoris has an increased pull on the tibial tuberosity. Hip flexion can be tested with the Thomas test, which can also be used to measure rectus femoris length (Deborah Roche, 2005). Gastrocnemius and soleus ROM is assessed via active and passive dorsiflexion. Normal values for dorsiflexion are between 0-20deg. Internal and external hip rotation is assessed with a lying prone test, with tested leg bent at 900(Deborah Roche, 2005), normal values for internal and external hip rotation seem to vary between literature, but normal values of 30-400deg for internal hip rotation and 40-600deg for external hip rotation are often quoted in literature (Robert P. Wilder, Francis C. O'Connor, and William Barrish, 2001). The IT band and tensor fascia latae can be tested with Ober test (Deborah Roche, 2005). Tightness in hip rotators is associated with a change in Q-angle, which will affect the proper knee biomechanics (Michael T Cibulka and Julie Threlkeld-Watkins, 2005, Naoko Aminaka, 2005).
The Q-angle is measured using a goniometer. This is done by first, placing the centre axis of a long arm goniometer over the centre of the patellar. Next, palpate the proximal tibia and align the lower goniometer arm along the patellar tendon to the tibial tubercle. Take the upper arm of the goniometer and point it directly at the anterior superior iliac spine. The small angle measured by the goniometer is the Q-angle (Mark Charrette, 2003). Best and most accurate results are yielded with the patients standing, as natural knee alignments with weight bearing is also being taken into account (Mark Charrette, 2003). Normal Q-angle in males is 11-17deg and 14-20deg in females. Tibial torsion evaluation is not very easy outside a clinical setting, and the tests show variable repeatability and accuracy (Milner CE and Soames RW, 1998). However, to assess tibial torsion, the examiner positions the medial and lateral femoral condyles in the frontal plane, and then palpates the medial and lateral malleoli. An imaginary axis between the medial and lateral malleoli is measured against the plane of the examining table, with normal values being between 15� to 25� of external tibial rotation (Robert P. Wilder, Francis C. O'Connor, and William Barrish, 2001). At this stage there is no point in testing quadriceps strength, as it can further irritate the injury and pre injury strength of the quadriceps is most likely not known. Hamstring strength should also not be tested, for the same reasons. The visual examination should be adequate to determine if any muscle atrophy of the quadriceps has taken. If the patient has both knees diagnosed with OSD, the patient should be asked to confirm any possible atrophy of the quads.
During the course of the treatment regular motion assessment should be performed, preferably every fortnightly, examining ROM, and pain symptoms. (Of course this will be mostly up to the patient, if they can make the time). If there is any doubt about the diagnosis or contradictory symptoms the patient should be asked to have some form of imaging, in order to dismiss any other possible knee pathologies, or to establish the stage of OSD, which is best done with MRI scans (Eric J. Wall, 1998, Atsushi Hirano et al., 2002).
The final stage in the client screening procedure is the functional tests. These are to determine the suspicions and assess severity of the injury (Perrin, D.H, 1999). A series of functional tests specific to OSD are:
- Is the tibia tuberosity tenderness to touch?
- Is there pain with straightening and bending of the injured knee, with active and passive, and resisted ROM?
- Bilateral comparison of the quadriceps and knee. Are they similar in strength and size?
- Can the patient jog straight ahead without pain and limping?
- Can the patient sprint straight ahead without pain and limping?
- Can the patient perform a 45-degree cut without pain?
- Can the patient perform a 90-degree cut without pain?
- Ability to do a 20-yard figure-of-eight run/s without pain or discomfort?
- Ability to do a 10-yard figure-of-eight run/s without pain or discomfort?
- Can the patient jump on both and injured leg without pain?
- Can the patient go up and down stairs without pain?
- Can the patient squat without pain?
(McKesson Health Solutions, 2004).
The evaluation of these test will be useful in determining the severity of the injury, stage of the injury treatment required he/she is in (acute, recovery, maintenance), and if patient is able to return to sport or no/or mild activity modification
The final step is to document and record all finding, and complete SOAP notes (Perrin, D.H, 1999)
Rehabilitation program
The rehabilitation program starts with determining the stage of OSD in the acute phase of the injury. This is done by comparing the results from the client screening, and the signs and symptoms outlined for each stage of OSD by Atsushi Hirano et al., (2002), or even better would be determination though MRI (Atsushi Hirano et al., 2002). Once the stage has been establish the best method of treatment can be decided upon. Regardless of stage, the first form of treatment will be at least a 4-8week rest period, with suspension of all activities that cause pain (such as running, jumping, squatting, and kicking), As well as regular icing for 20min several times a day. If complete rest is not an option, than regular cryotherapy for 20min, before and after trainings, and several times throughout the day, along with at least some activity limitations and the use of an infrapatellar strap is highly recommended (OJ Bloom, & Leslie Mackler, Barbee J. 2004). If pain and inflammation is persistent, or activity participation is not suspended, NSAID may be used, for short periods of time to help with inflammation (John. P. DiFiori, 1999). A hamstring, lower leg, and hip flexibility program may be commenced at this stage, without running a risk of further injury aggravation (David M. Peck, 1995). Exercise should be done on both sides, for injury prevention, and to counter-limb ROM balance
Acute Stage - Flexibility Program
| Exercise Sets | Duration | Frequency | |
| 1. Hamstring stretch on wall | 3-5 | 15-30sec | 2-3 times a day |
| 2. Standing Calf Stretch | 3-5 | 15-30sec 2-3 times a day | |
| 3. Standing Soleus stretch | 3-5 | 15-30sec | 2-3 times a day |
| 4. Iliotibial band, side leaning | 3-5 | 15-30sec | 2-3 times a day |
| 5. Hip Adductor Stretch | 3-5 | 15-30sec | 2-3 times a day |
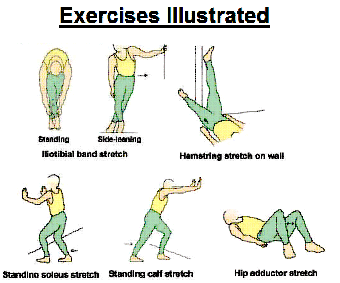
Iliotibial band stretch (side-leaning): Stand sideways near a wall, your injured leg toward the inside. Place the hand of the side closes to the wall for support. Cross your leg over, keeping the foot stable. Lean into the wall. (Tammy White, 2005)
Standing calf stretch: Facing a wall, put your hands against the wall at about eye level. Keep the injured leg back, the uninjured leg forward, and the heel of your injured leg on the floor. Turn your injured foot slightly inward (as if you were pigeon-toed) as you slowly lean into the wall until you feel a stretch in the back of your calf. (Tammy White, 2005)
Standing soleus stretch: Stand facing a wall with your hands at about chest level. With both knees slightly bent and the injured foot back, gently lean into the wall until you feel a stretch in your lower calf. Once again, angle the toes of your injured foot slightly inward and keep your heel down on the floor. (Tammy White, 2005)
Hip adductors stretch: Lie on your back, bend your knees, and put your feet flat on the floor. Gently spread your knees apart, stretching the muscles on the inside of your thigh. To increase the stretch, perform this stretch seated, with your heel together. You can hold your feet and to keep them as close to groin as you can. You push down on knees with your elbows for an ever greater stretch, this is called the butterfly stretch (caution must be paid not to push on the tibial tuberosity) (Tammy White, 2005)
Hamstring stretch on wall: Lie on your back with your buttocks close to a doorway, and extend your legs straight out in front of you along the floor. Raise the injured leg and rest it against the wall next to the door frame. Your other leg should extend through the doorway. You should feel a stretch in the back of your thigh. (Tammy White, 2004)
The desired outcome from this stage is to alleviate pain and inflammation, in order to commence a more comprehensive rehabilitation program. During the course of this rest period fortnightly physical exams are recommended in order to keep track of progress and variables such as height, and weight, which are used to keep track of growth rate (John P. DiFiori). These check-ups can also be used to continue to educate, support and motivate the patient, and help if need be, to cope with the effects of the injury. If after a full 8-week course conservative therapy the condition has not shown improvement, especially with treatment recommendations completely adhered too. It is highly advisable to have an imaging study to determine if ossicles formation is present. If the patient is old enough, and ossicles formation is detected, surgery may be the best treatment, for a speedy recovery with minimal loss of time, from training and sport participation (Engel A, Windhager R, 1987). If no ossicles are present conservative therapy treatment is still the treatment of choice until symptoms are alleviated.
When symptoms of pain and inflammation are alleviated, and maintained for a least 2 weeks the patient enters the recovery stage. In this stage of the rehabilitation program, stretching and strengthening exercises can be added for hamstrings and hip rotators (with the interest of normalising Q-angle) and stretching exercises for quads and calves. Once adequate flexibility in the quadriceps is established, strengthening exercise for the quad can be incorporated, to either restore normal quad girths (compared to uninjured leg) or atrophy due to decreased used. The main form of exercises are, pain-free isometrics, and low load high-repetition knee extension exercises. Progressive resistance exercise should be used with caution , as they may only increase pain at the tibial tuberosity (William E. Prentice & Michael I. Voight, 2001). Quadriceps stretches should focus on stretching the muscle belly, with little strain on the tibial tuberosity. (William E. Prentice & Michael I. Voight, 2001). Stretching exercises are first done prone with with single joint stretches, and then progress to two joint stretches while standing. (William E. Prentice & Michael I. Voight, 2001). The recovery stage can takes around 8 weeks, for the start of revascularization, healing, and ossification of the tibial tubercle to take place (Kathryn L. McCance & Sue E. Huether, 2002). It must be remembered that there is great variability between individuals, and healing times are only guidelines at best. The rehabilitation program is divided into 2. The first 4 weeks will be aimed at establishing extra quad length. If adequate flexibility is achieved and tension is reduced (which will hopefully be achieved within that 4 week period), than a more advanced stretching and strengthening program can be started. Increasing flexibility and reducing quadriceps pull on the tibial tuberosity is the primary goal, strengthening exercise are not as important, especially if there was no initial muscle atrophy prior to beginning the rehabilitation program.
Recovery Stage - Flexibility and Strength Program 1
Iliotibial band stretch (standing): Cross your one leg in front of the other and bend down and touch your toes. You can move your hands across the floor toward the one side and you will feel more of a stretch on the outside of your thigh. (Tammy White, 2005)
Prone hip extension: Lie on your stomach with your legs straight out behind you. Tighten up your buttocks muscles and lift one leg off the floor about 8 inches. Keep your knee straight. Hold for 5 seconds. Then lower your leg and relax. For a more advanced version exercise can be performed with both legs at the same time.(Tammy White, 2004)
Side-lying leg lift: Lying on your side, tighten the front thigh muscles on your leg and lift that leg 8 to 10 inches away from the other leg. Keep the leg straight, and do not tense so hard that it hurts or puts stress on the tibial tuberosity. (Tammy White, 2005)
Straight leg raises: Lie on the floor with the back propped up a few inches with the elbows. Bend the unaffected knee to a comfortable position. Using adjustable ankle weights with half-pound increments, determine the weight at which 10 raises can be performed on the affected leg. Tighten the thigh muscles and lift the affected leg 12 inches, keeping the leg straight. Hold for 5 seconds. Slowly lower the leg and relax. Start with 10 repetitions for each leg. When 15 repetitions have been performed comfortably, increase the weight by half a pound and drop back to 10 repetitions. Once 15 repetitions again can be performed comfortably, increase the weight again, to a maximum of 7-12 lb. 4 sets of 10 repetitions (Tammy White, 2004, Eric J. Wall, 1998)
Straight leg stretch using a towel: This is done the same as the hamstring stretch on wall, but a towel is used instead of the door. This way the patient can pull the leg back a little so they can go beyond 900 (Not illustrated).
Prone quad stretch: Lying face down on a table, with one knee bent. Using the hand on the same suide as the bent knee, reach back and grab your ankle. Pull the foot down towards your buttock. The stretch should be felt in the muscle belly, if stretch is felt in the tibial tuberosity, relax the stretch a little till a comfortable range is found.(not illustrated) (Robert C. Meisterling, Eric J. Wall, Michael R. Meisterling, 1998)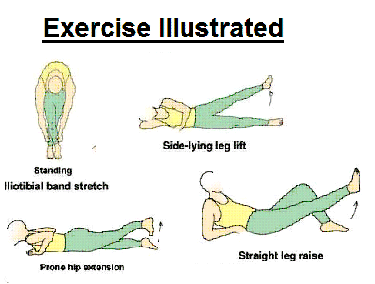
Recovery Stage - Flexibility and Strength Program 2
Hip abduction (with elastic tubing): Stand sideways near a doorway with your uninjured side closest to the door. Tie elastic tubing around the ankle on your injured side. Knot the other end of the tubing and close the knot in the door. Extend your leg out to the side, keeping your knee straight. Return to the starting position. To challenge yourself, move farther away from the door (Tammy White, 2005)
Supine quad stretch: Laying supine on a table with the buttocks of the to be stretched leg hanging over the edge. Let the knee bend down , with the same arm as leg, grasp the ankle and pull it down and back (as illustrated). A stretch in the quad and the front of the hips should be felt. (R.P. Jakob, S. Von Gumppenberg, and P Engelhardt, 1989)
Short-arc quadriceps exercises: Lay back with the unaffected knee bent (same as for straight leg raises).Place a few rolled up towels under the affected knee to raise it 6 inches from the floor. Tighten the thigh muscles and straighten the leg until it is 12 inches from the floor. Hold for 5 seconds. Slowly lower the leg and relax. Using the same ankle weight and repetition progression as for straight leg rises. (Robert C. Meisterling, Eric J. Wall, Michael R. Meisterling, 1998)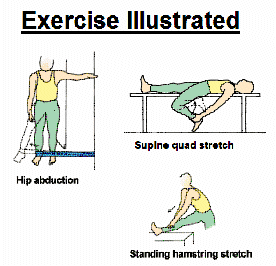
During the course of the recovery program, regular fortnightly check-ups are recommended, to assess functional activity, and to once again aid in the adherence to the program. It is advised that during this stage the patient be involved in his sport in some form. He/she should also undertake an alternative method of cardiovascular training, in order to reduce detraining effects (William E. Prentice & Michael I. Voight, 2001). Reasonable alternatives are hand ergometer training, and or possibly swimming (aqua therapy). A specific cardiovascular program should be devised with the aid of the exercise physiologist and coach, to best maintain or possibly in improve cardiovascular fitness during the course of the rehabilitation program (William E. Prentice & Michael I. Voight, 2001). Aqua therapy exercise as a means of rehabilitation for OSD has not been studied from knowledge of the author, thus possible use of aqua therapy exercise for maintenance of motor skills and rehabilitation of OSD patients is unknown. After the 8th weeks,if the patient is showing a good prognosis he or she may be ready to return to sport.
Return to sport is evaluated via response to functional tests, which were and should be performed at the initial screening and periodically during the rehabilitation program stages. The use of certain sport specific motor skills can also a good evaluation tool (attempted in progressive manner, from easiest to hardest) (William E. Prentice & Michael I. Voight, 2001, Perrin, D.H, 1999). If client is able to perform all functional test, and motor skills with full power, full effectiveness, and full aggressiveness, unrestricted by fear of the injury worsening, than he/she is ready to return to sport training, and eventually competition. (K. Dean Reeves et al. 2006). Once the client is evaluated as being fit to return to training, the maintenance stage of rehabilitation is entered. During this stage sports training and participation is resumed (progressively), and a maintenance program involving more complex and sport specific exercises is empoyed. These exercises should be performed during team trainings, under the supervision of the coach. This will help the athlete re-establish his/her place in the team or sport, and gain confidence back to return to competition. The chance of adherence is also increased, as he/she has constant supervision. (Larry Nassar, 2000). Exercise recommendations:
- Progressive, from simple to complex >
- Single to multi joint exercises, skills or drills
- Maintenance of quadriceps and hamstring flexibility
- Maintenance of hip flexibility and ROM.
- A greater emphasis on functional exercises.
- From an overprotective environment to a more realistic competition environment
Maintenance Stage Program
Wall slide: To do wall slides or quarter seats, stand about 12 inches from a smooth wall and lean back against it with the feet shoulder width apart (a swiss-ball can also be used to lean on, to facilitate smooth motion). Holding a light dumbbell in each hand with the arms straight down, bend the knees and slowly lower the body 4-6 inches. If pain is felt, the body has squatted too far. Hold for 5 seconds and then rise up quickly. Start with 10 repetitions and increase to 15, gradually increasing the dumbbell weight in the same type of progression as for straight leg raises. Later, can progress to single leg wall slides. It is performed the same way as above, but keep the unaffected leg about and inch of the floor and you slide, squat, and straighten up. Robert C. Meisterling, Eric J. Wall, Michael R. Meisterling, 1998
Rope Jumping: Stat with 1 min and progress to 5min with 10sec increments every session. Robert C. Meisterling, Eric J. Wall, Michael R. Meisterling, 1998
Side to side runs: Running laterally for 20m in one direction, joining the feet together before separating again. And than 20m in the other direction. Runs should be lateral in a straight line.
Standing quad stretch: Same as in supine, but standing on one leg. A contact surface can be used for support initially.( R.P. Jakob, S. Von Gumppenberg, and P Engelhardt, 1989)
If the maintenance phase of rehabilitation is achieved, long term adherence of no less than 6months and preferably up to the age of 18 is recommended. At this age the apophysis and apophysis have closed. Until this age, caution is still advised against overstressing the tibial tuberosity, though trainings, and up keeping at least some form of quadriceps and hamstring stretching and strengthening exercise program.
Reference:
- Munisha Mehra Bhatia (2004). Osgood-Schlatter Disease, Emedicine [e-journal] http://www.emedicine.com/sports/topic89.htm, date accessed: Jul 13 2004
- Atsushi Hirano, Toru Fukubayashi, Tomoo Ishii, Naoyuki Ochiai. (2002) 'Magnetic resonance imaging of Osgood-Schlatter disease: the course of the disease'. Skeletal Radiology, Vol 31; 334-342
- Antonio Gigante, Claudia Bevilacqua, Massimo G Bonetti & Francesco Greco (2003) 'Increased external tibial torsion in Osgood-Schlatter disease'. Acta Orthopaedica Scandinavica, Vol. 74 No.4; 431-436
- Kazunari Ishida, Ryosuke Kuroda, Keizo Sato, Tetsuhiro Iguchi, Minoru Doita, Masahiro Kurosaka, & Tetsuji Yamamoto (2005) 'Infrapatellar Bursal Osteochondromatosis Associated with Unresolved Osgood-Schlatter Disease'. Journal of Bone and Join Surgery, Vol. 87 No.12; 2780-2783
- Sue E. Huether & Kathryn L. McCance (2004) Understanding Pathophysiology; Missouri St Louise; Mosby.
- L. Pearce McCarty III (2005). 'Treating patients with patellofemoral conditions--Most can be managed nonoperatively'. The Journal of Musculoskeletal Medicine, Vol. 22; 667-673
- McKesson Health Solutions (2004).'Osgood-Schlatter Disease'. Pediatric Advisor. Jan 1. 2270.
- Carl V Gisolfi & David R. Lamb (1989). Prespectives in Exercise Science and Sport Medicine, Volume 2: Youth Exercise and Sport. Indianapolis, USA : Cooper Publishing Group, LLC.
- James F. Dunn Jr. (1990) 'Osgood-Schlatter disease'. American Family Physician, Vol.41, No.1; 173(4). _NOT USED!!!
- Eric J. Wall (1998).' Osgood- Schlatter Disease; Practical Treatment for a Self-Limiting Condition'. The Physician and Sportsmedicine. Vol.26, Iss. 3; 29
- Cliggot Publishing Co. (2001). Consultant, Vol 41, Iss 10; 1479
- William E. Prentice & Michael I. Voight, (2001). Techniques in Musculoskeletal Rehabilitation. New York: McGraw Hill
- Leslie Klenerman (1994). 'Musculoskeletal injuries in child athletes (ABC of sport medicine)'. British Medical Journal. Vol 308, No. 6943 ; 1556(4)
- David M. Peck (1995).' Apophyseal injuries in young athletes'. American Family Physician. Vol. 51, No. 8; 1891(7)
- OJ Bloom, & Leslie Mackler, Barbee J. (2004)'What is the best treatment for Osgood-Schlatter Disease?'.The journal of family practice. Vol. 53, No. 2.
- John. P. DiDiori. (1999)'Overuse injuries in children and adolescents'. The Physician and Sportsmedicine. Vol 27, Iss. 1; pg75
- Walter L. Calmbach & Mark Hutchens (2003).'Evaluation of Patients Presenting with Knee Pain: Part II. Differential Diagnosis. American Family Physician. Vol.23, No.9: 917-922
- Sheila Globus (2002).'Osgood-Schlatter: More than growing pains. Current Health 2. Stamford. Vol. 28, Iss. 5; 20
- Gregory S. Kolt & Lynn Snyder-Mackler (2003). Physical Therapies in Sport and Exercise. London; Churchill Livingstone
- R.P. Jakob, S. Von Gumppenberg, and P Engelhardt (1989).'Does Osgood-Schlatter Disease Influence the Position of the Patella'. The Journal of Bone and Joint Surgery.Vol.63-B, No. 4, 579-582
- H. Ware (1996).'Injury to the extensor mechanism in the knee'. The Knee. Vol. 3 Iss. 1; 94(2)
- Graf BK. Fujisaki CK, Reider B, 1991),'Disorders of the patellar tendon' in: Reider B, ed.. Sport Medicine: The school aged Athlete. Philladelphia, Saunders, 1991. p355
- Kujala UM, Kvist M, Heinonen O (1985) Osgood-Schlatter Disease in Adolescent Athletes: 'Retrospective study of incidence and duration. American journal of Sport Medicine. Vol.13 :239
- Hiroshi Ikeda, Hisashi Kurosawa, Keishoku Sakuraba, Hauyasu Ohta and SunGon Kim (1999).'Analysis of quadriceps muscle strength and tension in adolescent athletes with Osgood-Schlatter disease. Journal of Orthopedic Surgery. Vol 7, Iss.1; 27-31
- M.S. Turner, I.S. Smillie, (1981).'The Effect of Tibial Torsion on the Pathology of the Knee'.The Journal of Bone and Joint Surgery. Vol.63-B, No.3 396-398
- Debera Brodwell Jackson, Rebecca B. Saunders (1993).'Child Health Nursing: A comprehensive approach to care of children and their families; Philadelphia: Lippincott Company
- Kathryn L. McCance & Sue Heather, (2002) Antrophysiology: The Biologic Basis for Disease in Adults & Children; St. Louis: Mosby
- Dr Emma Lackey and Dr Ron Sutton (2006).'Clinical: Rest is the best treatment for common knee swelling. GP. Feb 17, 2006, p30
- G.S. Dowd (1996).' Anterior knee pain'. The Knee. Vol 3. Iss. 1:98(2)
- D.Barbuti, C Orazi, G. Bergami, (1995)'Sonography of the knee in pediatric age: our experience'. European Journal of Utrasound. Vol.2, Iss. 2:p1(1)
- Steven I. Subotnick (1977). The running foot doctor; California: World Publications
- Robert C. Meisterling, MD, Eric J. Wall, MD, Michael R. Meisterling, (1998).'Coping with Osgood-Schlatter Disease. The Physician and Sportsmedicine. Vol.26, Iss.3; pg39
- Viktoras Gerulis, Romas Kalesinskas, Sigitas Pranckevicius, Paulius Bergeris, (2004)' Importance of conservative treatment and physical load restriction to the course of Osgood-Schlatter's disease'.Medicina. Vol 40, No. 4:pg363-369
- Tammy White. (2004). Osgood-Schlatter disease Rehabilitation Exercises. Clinical Reference Systems. McKesson Health Solutions LLC. Jan 1, 2004, p2296
- K. Dean Reeves, Brad Fullerton, Gaston Topol, and Greg Bancroft (2006) 'Study seeks treatment to keep athletes in the game: The effects of Osgood-Schlatter disease can extend beyond resolution of pain to a patient's sports career'. BioMechanics Magazine Online [e-magazine] http://www.biomech.com/showArticle.jhtml?articleID=185302966. April 2006 issue. Date accessed: 7.5.06
- Reeves KD, Hassanein KM (2003).' Long-term effects of dextrose prolotherapy for anterior cruciate ligament laxity: a prospective and consecutive patient study'. Alternative Therapies in Health and Medicine. Vol. 9(3):58-62.
- Deborah Roche (2005). 'Guidelines for Athlete Assessment in New Zealand Sport: Flexibility and Muscle Balance Assessment'. Sport Science New Zealand.
- Eric Shamus & Jennifer Shamus, (2001). Sports Injury Prevention & Rehabilitation. USA; The McGraw-Hill Companies
- Freddie H. Fu & David A. Stone (1994). Sport Injuries: Mechanisms, Prevention, Treatment. Baltimore, Maryland; William & Wilkins
- Springhouse publishing company (2005) Professional guide to diseases. Pennsylvania; Lippincott Williams and Wilkings
- Steven J. Anderson (1991).' Overuse injuries in young athletes'. The Physician and Sportsmedicine. Vol.19 No.12: p69(9)
- Timothy Floyd, George D. Picetti III, Richard Schneider (1989).'Tibial tubercle avulsion'. The Physician and Sportsmedicine. Vol. 17, No.8; p79(3)
- Kathryn L. McCance and Sue E. Huether (2002) Antrophysiology: The Biologic Basis for Disease in Adults & Children; St. Louise: Mosby
- Dorathy R. Marlow, Barbara A. Redding (1988).6th Edition,'Textbook of paediatric nursing', Philadelphia: W.B. Saunders Company.
- Michael D. Ross, and Douglas Villard (2003).'Disability levels of collage-aged men with a history of Osgood-Schlatter's disease'. Journal of Strength and Conditioning research. Vol.17 Iss.4: Pg 659(5)
- Medical multimedia group (2005).'A patient's Guide to Osgood-Schlatter Lesion of the Knee". eOrthopod [ http://www.eorthopod.com/eorthopodV2/index.php/fuseaction/topics.detail/ID/1e69153b4390c6eff3095daeefe6031a/TopicID/9c2c5ae2333ff1b24f5fb4a3abba8184/area/46 ]. Date accessed 23.05.2006.
- Beckman, M.; Craig, R.; Lehman, R.C (1989). "Rehabilitation of patellofemoral dysfunction in the athletes." Clinics in Sports Medicine; Vol. (8)4, Oct: pg841-860.
- David Edell (2005). Osgood-Schaltters. http://www.athleticadvisor.com/Injuries/LE/Knee/osgood-schlatters.htm [URL].Date accessed: 23.05.06, last update 04/19/05
- Naoko Aminaka; Phillip A. Gribble (2005).'A systematic review of the Effects of Therapeutic Taping on Patellofemoral pain syndrome'. Journal of Athletic Training. Vol. 40(4): pg 341-351
- Rosalind Coombs and Gerard Garbutt, (2002).' Developments in the use of the hamstraing/quadriceps ratio for the assessment of muscle balance'. Journal of sport science and medicine. Vol.1: Pg 56-62
- M.G.E. Peterson, M. Murray-Weir, L Root, M. Lenhoff, L. Daly, C. Wagner, (2000.)"Bootstrapping Gait Data from People with Cerebral Palsy," cbms, p. 57, 13th IEEE Symposium on Computer-Based Medical Systems (CBMS'00),
- Perrin, D.H (1999). The evaluation process in the rehabilitation. (in:W.E Prenctice, 1999. Rehabilitation techniques in sports medicine. 3rd ed. Boston: McGraw-Hill. p.607)
- Milner CE and Soames RW (1998).' A comparison of four vivo methods of measuring tibial torsion". Journal of Anatomy . Jul, 193(pt 1):139-44
- Mark Charrette (2003). 'Abnormal Q-angle and Orthotic support'. Dynamic Chiropractic. Vol.21 Issue 24.
- Christopher C. Madden & Morris B. Mellion (1996).'Severs disease and other causes of heel pain in Adolescents'. American Family Physician. Vol.54 No.6: pg1995-2000.
- Michael T Cibulka and Julie Threlkeld-Watkins (2005).' Patellofemoral Pain and Asymmetrical Hip Rotation'. Journal of the American Physiotherapy Association. Vol. 85 No. 11: pg
- Marlene A. Prost (2002).' IN THE GAME: Pinpointing biomechanical faults can keep athletes on their feet'. Advance for Directors in Rehabilitation. Vol.11, Iss.5: pg41
- Robert P. Wilder, MD, Francis C. O'Connor, MD, and William Barrish, MD, (2001).'Picking up the pace: revitalise runners with the right diagnosis'. BioMechanics Magazine Online [e-magazine] http://www.biomech.com/db_area/archives/2001/0109.cover.bio.shtml. September 2001 issue. Date accessed: 7.5.06
- Engel A, Windhager R, (1987)'. Importance of the ossicle and therapy of Osgood-Schlatter disease'. Sportverletz Sportschaden. Vol. 1(2), June: pg 100-8
- Tammy White (2005). Sport Medicine Advisor 2005.4: Iliotibial Band Syndrome Rehabilitation Exercises. McKesson Provider Technologies. Date accessed: 21.5.06 [http://www.med.umich.edu/1libr/sma/sma_knee-ili_rex.htm]
- Tammy White (2005). Sport Medicine Advisor 2005.4: Ankle Sprain Rehabilitation Exercises. McKesson Provider Technologies. Date accessed: 21.5.06 [http://www.med.umich.edu/1libr/sma/sma_anksprai_rex.htm]
- Tammy White (2005). Sport Medicine Advisor 2005.4: Groin Sprain Rehabilitation Exercises. McKesson Provider Technologies. Date accessed: 21.5.06 [http://www.med.umich.edu/1libr/sma/sma_groinstr_rex.htm
- Larry Nassar (2000)' Coaches Medical Primer: U.S.E.C.A Elite Gymnastics Video #135, DVD, 120min
By Valentin-Angelo T. Uzunov.
